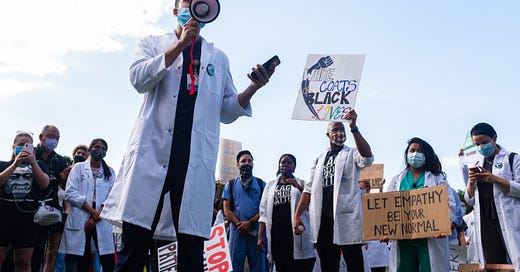The Hypocritical Oath
Doctors should not pretend that they are experts in how society should be run.

Is Tech Changing the World for Better or Worse? Please join us today, from 3pm Eastern Time, for a debate about the impact digital technology is having on the future of politics with two of the most interesting thinkers in this space, Cathy O’Neill and Martin Gurri.
There have been a growing number of calls for doctors to make the fight against racism central to what they do. The American Board of Internal Medicine, for example, recently decried “structural, systemic and cultural racism.” Meanwhile, the American Academy of Pediatrics has implored its members to “dismantle racism at every level” of society.
Their logic is straightforward. Living in a racist society and being exposed to racist police violence is bad for the health of black Americans. Doctors should thus do three things: increase diversity within the medical profession, improve their understanding of the social determinants of health, and contend with broad social issues that impact health in a less direct manner.
The first two of these aims are laudable. But the third takes physicians into realms where they have no expertise—and thus risks eroding public trust in the medical profession.
Only five percent of physicians are black. This leaves many black students without role models and mentors of their own race. A high proportion of black faculty members also report feeling isolated and undervalued, or being passed over for promotion. Since the late 1960s, medical schools have tried to address these problems by increasing the racial diversity of their faculty and students—hoping that this would also broaden access to quality health care, since minority students are more likely to practice in underserved areas.
But even if a greater number of doctors belonged to ethnic minorities, and underserved communities could access better health care, disparities between racial groups would not necessarily disappear because other vulnerabilities cluster by group. Black people are, for example, three times more likely to be infected by the coronavirus than white people. This differential attests to the role of non-medical factors in health—in this case, the increased risk of exposure that comes from employment as essential workers, a greater dependence on public transportation, and residency in higher density accommodation and neighborhoods.
Medical schools therefore familiarize trainees with various ways of influencing the social determinants of health. In one model, for example, community health workers help low-income patients suffering from chronic conditions to access affordable childcare, job training and nutrition programs.
Childcare and food pantries may not sound like conventional medical care. But attending to patients’ social needs has a long and proud history within medicine. Doctors can better serve patients when they appreciate the complexities of their lives—I myself have, for example, drawn on my experiences as a psychiatrist to lobby for jail diversion programs to treat addicted offenders.
What makes such involvement appropriate for physicians is its closeness to the orbit of care. Promoting access to health care, for example, makes eminent sense for a profession that exists to provide such care.
Still, matters can get murky when physicians promote particular policies to achieve their goals. The American Medical Association would politicize the profession if it advocated, for instance, a single payer health system.
I fully support increasing diversity within the medical profession and addressing the social conditions that directly impact health, then. But I am deeply concerned about the third demand that activists are now making of my field: that we should advocate for causes that are, at best, only remotely connected with health—and which physicians have no special expertise to address.
In 2001, the American Medical Association adopted a Declaration of Professional Responsibility that encourages doctors to “advocate for social, economic, educational, and political changes that ameliorate suffering and contribute to human well-being.” At the time, the declaration received little attention. But this began to shift when White Coats For Black Lives (WC4BL), a medical student organization, gained momentum. Founded in 2014 in response to the deaths of Michael Brown and Eric Garner, this organization now has chapters in over 30 medical schools, including Columbia, Stanford and the University of Chicago. A major plank of its platform is that “policing is incompatible with health.” (The visibility of WC4BL took off after the killing of George Floyd this May.)
The tendency to take explicit and radical stances on issues that are, at best, indirectly connected to questions of public health is also increasingly common among the medical establishment at large. Consider a recent essay by Donald M. Berwick MD, a former director of the Centers for Medicare and Medicaid, in the Journal of the American Medical Association. Dr. Berwick’s “agenda for action” includes doctor-led support for ratification of human rights treaties and opposition to the electoral college.
With the activist imperative comes a new teaching paradigm. Stanford University School of Medicine, for example, has just published an “anti-racist” curriculum, which instructs students in “confronting white supremacy.” The University of California at San Francisco offers a “toolkit” for “anti-racism and race literacy,” which emphasizes “white privilege” and recommends Robin DiAngelo’s White Fragility. The Association of American Medical Colleges wants schools to administer “unconscious bias training”; Michigan Governor Gretchen Whitmer has even signed an Executive Directive to develop rules that require implicit bias training for health professionals.
Strikingly few educators seem concerned about the implications of such pedagogy. Will the politicized “anti-racist” classroom be able to summon the neutrality needed to impart scholarly findings of rigorous medical sociology? Will instructors encourage civil debate and viewpoint diversity? How will they treat students who disagree that our political economy is “predicated on devaluing Black labor, demeaning Black bodies, and denying Black humanity”? And how can we effectively promote the importance of self-care—following a diet, exercising, taking prescribed medications regularly—under a regime that sees patients as being almost exclusively at the mercy of social forces?
These worries are compounded by the fact that two staples of anti-racism that are now at the heart of the successor medical curriculum are, at best, scientifically dubious. Implicit bias trainings aim to make people aware of their unconscious racial prejudices so that they can curtail any discriminatory practices in the future. But a sizeable body of research casts significant doubt on their ability to change behavior. For while the phenomenon of unconscious bias is very real, the Implicit Association Test, the tool used to measure such bias, can yield individual test results that vary significantly from day to day. Even when they don’t, those who are shown to have stronger bias do not seem to act in a more biased manner in real inter-personal situations.
The thesis of White Fragility is equally questionable. A key premise of DiAngelo’s book is that white people are both racist and cannot tolerate admitting that they are. Worse, no white person can present evidence to the contrary, since any attempt to do so would simply betray their unconscious determination to perpetuate white supremacy: “White fragility is not weakness per se,” she writes. “In fact, it is a powerful means of white racial control and the protection of white advantage.”
This idea has rightly been decried as unscientific. By asserting that a white person’s very denial of his or her racism constitutes proof of that racism, DiAngelo violates the fundamental scientific principle of falsifiability. Such an inept standard of evidence would be unacceptable in other medical school courses such as physiology, neuroscience and pathology; and yet, it is now in the ascendant at many medical schools.
Doctors learn a lot during their training. But they should not spend their time in medical school being told how to re-order, for example, an unfair economic system. Our empathy for victims of unfairness ought to reach that far—but our expertise doesn’t and can’t. As Dr. Farr A. Curlin, a professor of medical humanities at Duke University, has recently put it, “we are not authorities on all the complexities of a rightly ordered family, city, nation and world. The public would see through this bald pretense, and grow more skeptical … about what medical professionals say.”
Doctors who want to influence electoral politics or promote immigration reform should of course feel empowered to do so as private citizens. But, just as importantly, they should not feel pressured to become active in politics, or to adopt specific views on the nature of race relations.
Racism is indeed a poison. But physicians are not trained to extract it from the body politic. And if doctors stretch their authority too far, it will break.
Sally Satel MD is a Visiting Professor of Psychiatry at Columbia University’s Vagelos College of Physicians and Surgeons and a resident scholar at the American Enterprise Institute.